Acute Pancreatitis
content of this page
1- Introduction
2- Anatomical Overview
3- Treatment
4- purposes
Introduction
Acute pancreatitis is a condition characterized by the sudden inflammation of the pancreas, a gland located behind the stomach that plays a crucial role in digestion. The inflammation occurs when digestive enzymes become prematurely activated within the pancreas, causing damage to pancreatic tissue and leading to a cascade of inflammatory responses.
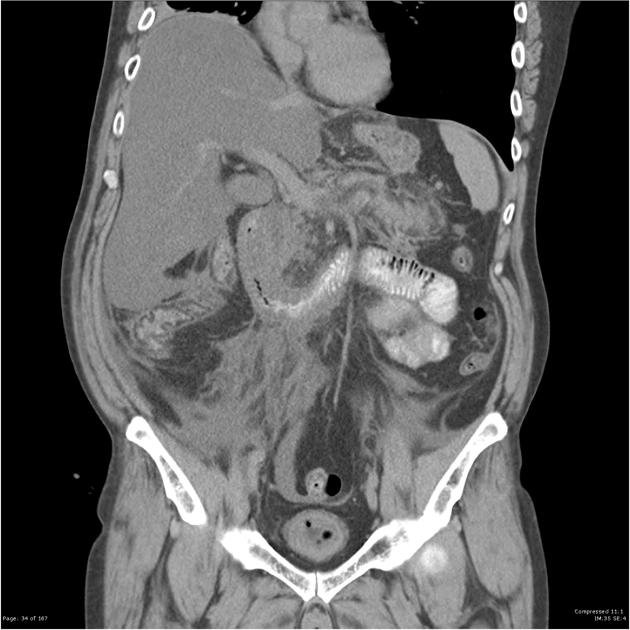
Anatomical Overview
The pancreas has a complex anatomy, consisting of a head, body, and tail. The head of the pancreas is nestled within the curve of the duodenum (the first part of the small intestine) and is connected to the bile duct, which carries bile from the liver and gallbladder. The body of the pancreas extends towards the left side of the abdomen, behind the stomach, and the tail reaches towards the spleen on the left side.
The pathophysiology of acute pancreatitis involves the abnormal activation of digestive enzymes within the pancreas. Normally, these enzymes are produced in an inactive form and become active only when they reach the small intestine. However, in acute pancreatitis, these enzymes become prematurely activated within the pancreas, leading to auto-digestion and tissue damage. This process triggers an inflammatory response, causing swelling, cell injury, and disruption of blood flow within the pancreas.
Acute pancreatitis can be caused by various factors, including gallstones, alcohol consumption, infections, medications, and trauma. Gallstones are a common cause, as they can block the pancreatic duct, leading to enzyme buildup and inflammation. Alcohol consumption can directly damage pancreatic cells and trigger inflammation.
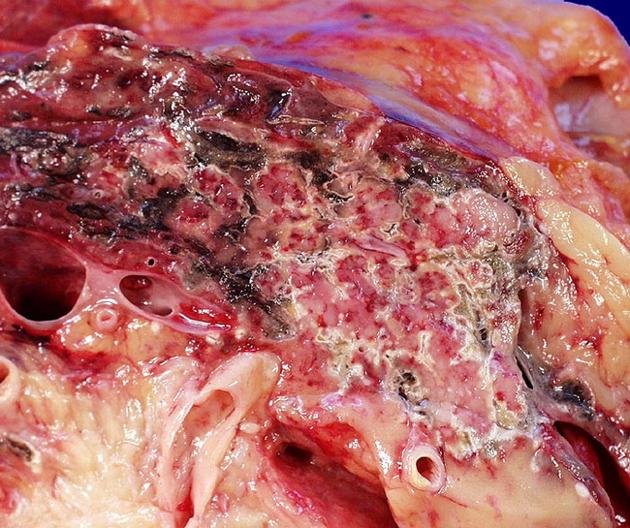
Treatment
Mild Acute Pancreatitis:
- Hospitalization: Some cases may require hospitalization for monitoring and supportive care.
- Fasting: To give the pancreas time to rest and recover, the patient may be kept NPO (nothing by mouth) initially.
- Pain Management: Medications such as acetaminophen or opioids can help manage pain.
Severe Acute Pancreatitis:
- IV Fluids: Intravenous fluids are given to prevent dehydration and maintain electrolyte balance.
- Nutritional Support: If the patient cannot eat, nutrition may be provided through a feeding tube.
- Antibiotics: If there is evidence of infection, antibiotics may be prescribed.
- ERCP (Endoscopic Retrograde Cholangiopancreatography): If gallstones are causing the pancreatitis, ERCP may be performed to remove them.
- Surgery: In severe cases, surgery may be needed to remove damaged tissue or treat complications such as pseudocysts or necrosis.
Complications Management:
- Pseudocysts: Fluid-filled sacs that may form in or around the pancreas may require drainage.
- Necrosis: Dead tissue in the pancreas may need to be removed surgically.
- Organ Failure: Intensive care may be needed to support organ function.
Purposes
-
Relieve Symptoms: Alleviate the severe abdominal pain, nausea, vomiting, and fever associated with acute pancreatitis to improve the patient’s comfort and well-being.
-
Prevent Complications: Address underlying causes such as gallstones or alcohol abuse to prevent complications such as pseudocysts, necrosis, or organ failure.
-
Promote Healing: Provide supportive care, including fasting and intravenous fluids, to rest the pancreas and allow it to recover from inflammation and injury.
-
Manage Infection: Administer antibiotics if there is evidence of infection to prevent the spread of infection and further damage to the pancreas.
-
Address Underlying Causes: Perform procedures such as ERCP to remove gallstones or surgical intervention to treat complications like pseudocysts or necrosis.
-
Prevent Recurrence: Educate patients about lifestyle changes, such as avoiding alcohol and maintaining a healthy diet, to reduce the risk of future episodes of acute pancreatitis.